Share
Glaucoma is known to be one of the leading causes of irreversible vision loss worldwide, and while there is no cure for this disease, the risk of vision loss can be minimised through early diagnosis and management.1,2 Most cases of glaucoma have no symptoms, which means the condition can only be detected through a routine eye exam, most commonly performed by an optometrist.1,2
After being diagnosed with glaucoma, it is normal to feel overwhelmed and confused by the different eye health professionals you need to have ongoing appointments with. In this article, I will explain an optometrist’s role in your circle of care and how we work closely with ophthalmologists to provide the best care and vision outcomes.
What’s the difference between an optometrist and an ophthalmologist?
An optometrist is usually the first person you see when you have a routine eye test. They offer a wide range of eye care services, including assessing whether you need glasses by determining your prescription. During an eye test, optometrists’ can also detect eye conditions using specialialised equipment and technology that looks closely at the different parts of your eye. Some optometrists have a therapeutic endorsement, meaning they have completed additional training that allows them to prescribe certain ocular medications (such as eye drops and ointments).1
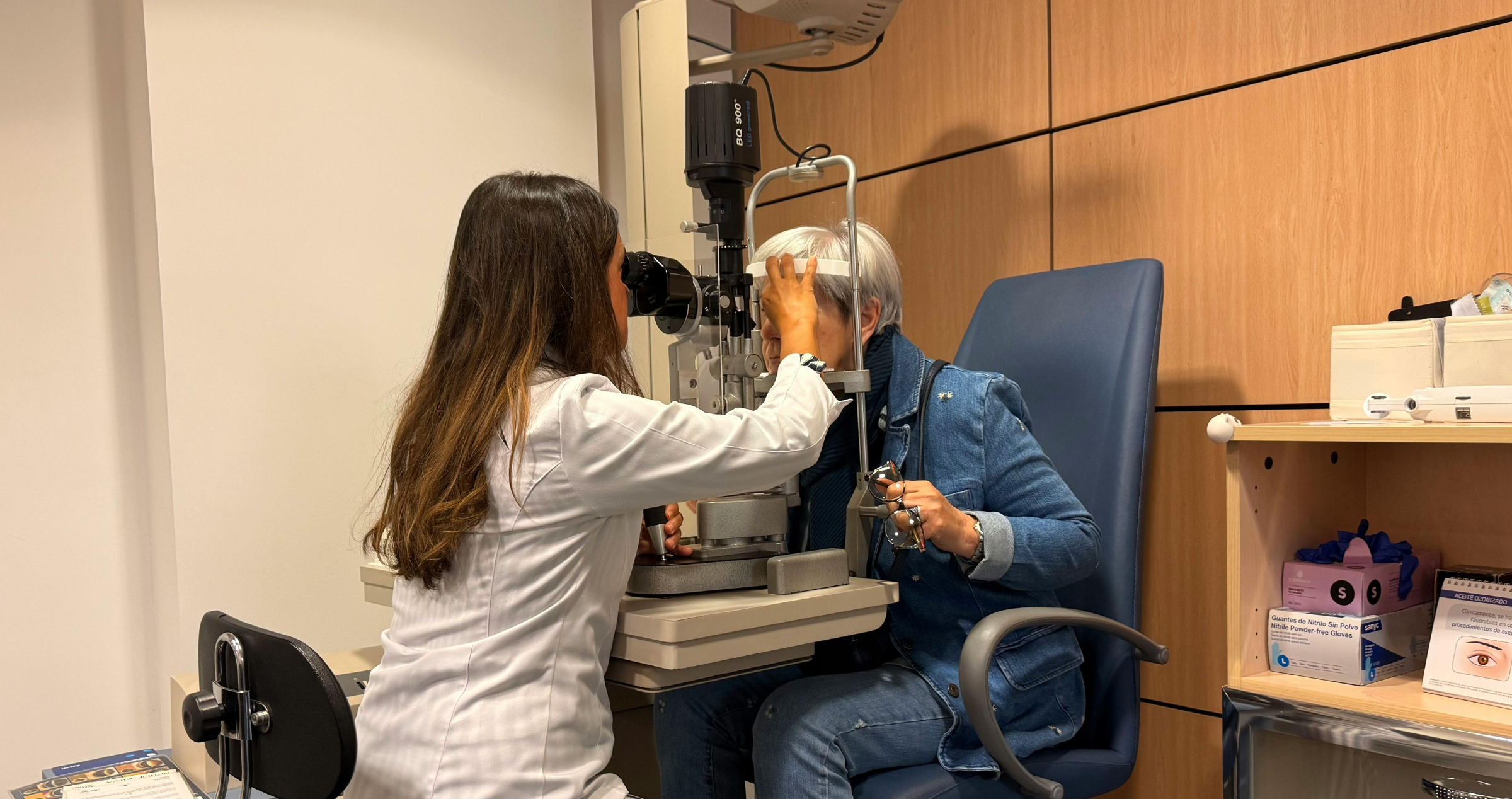
In the case of glaucoma, an optometrist is often the first eye care professional to detect glaucoma due to its lack of noticeable symptoms.1,3 During the eye test, an optometrist will assess risk factors and examine the structures within the eye, the optic nerve and eye pressures. They may also check your peripheral vision with a visual fields test and perform an OCT scan on your optic nerve.
If the optometrist suspects that you may have glaucoma, they will recommend and arrange a referral to an ophthalmologist for further assessment and confirmation of the diagnosis. An ophthalmologist is a medical specialist trained in the diagnosis, treatment and management of eye diseases and disorders. They are qualified to prescribe medications and perform eye surgeries. In some cases, when the eye pressure is elevated, your optometrist may initiate glaucoma management (usually in the form of eye drops) prior to the referral.1,3 If a patient is referred to a public ophthalmology clinic, they may experience a waiting period before receiving an appointment. In this situation, it is best for your optometrist to continue performing eye tests and monitoring you for progression while you wait.
Do I still need to see an optometrist if I am seeing an ophthalmologist?
When a patient is cared for by multiple health professionals working together, it is referred to as collaborative care. This form of care is very common when managing glaucoma patients due to the need for ongoing monitoring over a patient's lifetime.1 This model of care typically involves an optometrist, an ophthalmologist and a general practitioner.1 Depending on the type of test, check-up or treatment option required, you will have an appointment booked with a different professional in your collaborative care circle, with everyone kept informed of progress and changes to your management plan, so they can continue to work effectively together.1
In conclusion, managing glaucoma requires a collaborative approach, with optometrists playing an important and central role in the early detection, ongoing monitoring and care of this chronic eye condition. While ophthalmologists are vital for diagnosing and treating glaucoma, optometrists are often the first to identify it and provide essential ongoing support through regular eye examinations.
By working closely with ophthalmologists and other health professionals, optometrists help ensure that patients with glaucoma receive comprehensive care and optimal vision outcomes. Regular check-ups with your optometrist are vital, particularly for those with a family history of glaucoma1,2, as early detection and consistent monitoring can significantly reduce the risk of irreversible vision loss.
Ultimately, maintaining an open line of communication among your healthcare providers is key to effectively managing glaucoma and preserving your eye health throughout life.
References:
Glaucoma Australia. What is glaucoma?. 2025. Accessed June 27, 2025. https://glaucoma.org.au/
Vision Australia. Glaucoma. 2025. Accessed June 27, 2025. https://www.visionaustralia.org/services/eye-conditions/glaucoma
Wood J, Jeffery M, Tame S. Glaucoma screening by optometrists. Clinical and Experimental Optometry. 2021;76(6):199-207. https://doi.org/10.1111/j.1444-0938.1993.tb03058.x




